

Welcome to Diabetes Prevention Thursdays! Today, let’s talk about some basic reminders for caring for type two diabetes (T2D) at home. Maybe you or a loved one was just diagnosed with T2D. Or perhaps you’ve been struggling with it for years. Either way, it’s hard to be diagnosed with a chronic condition. It changes your psychological landscape, and keeping the condition under control seems impossible. Truthfully, insulin resistance is reversible and manageable through simple changes that can also prevent complications.
Quick Basics
T2D is a lifelong condition where cell receptors become resistant to insulin even though the pancreas continues to produce it. Pancreatic beta cells release insulin to allow other cells in your body to collect, convert, and store energy. The cells in the liver and muscles have a layer of mitochondria that exposes itself through insulin absorption, and it turns carbohydrates into glucose. With too many carbs, the cells become overworked, but the pancreas continues to produce insulin. Eventually, the mitochondria stop functioning as they should.
Tracking Your Blood Glucose Levels
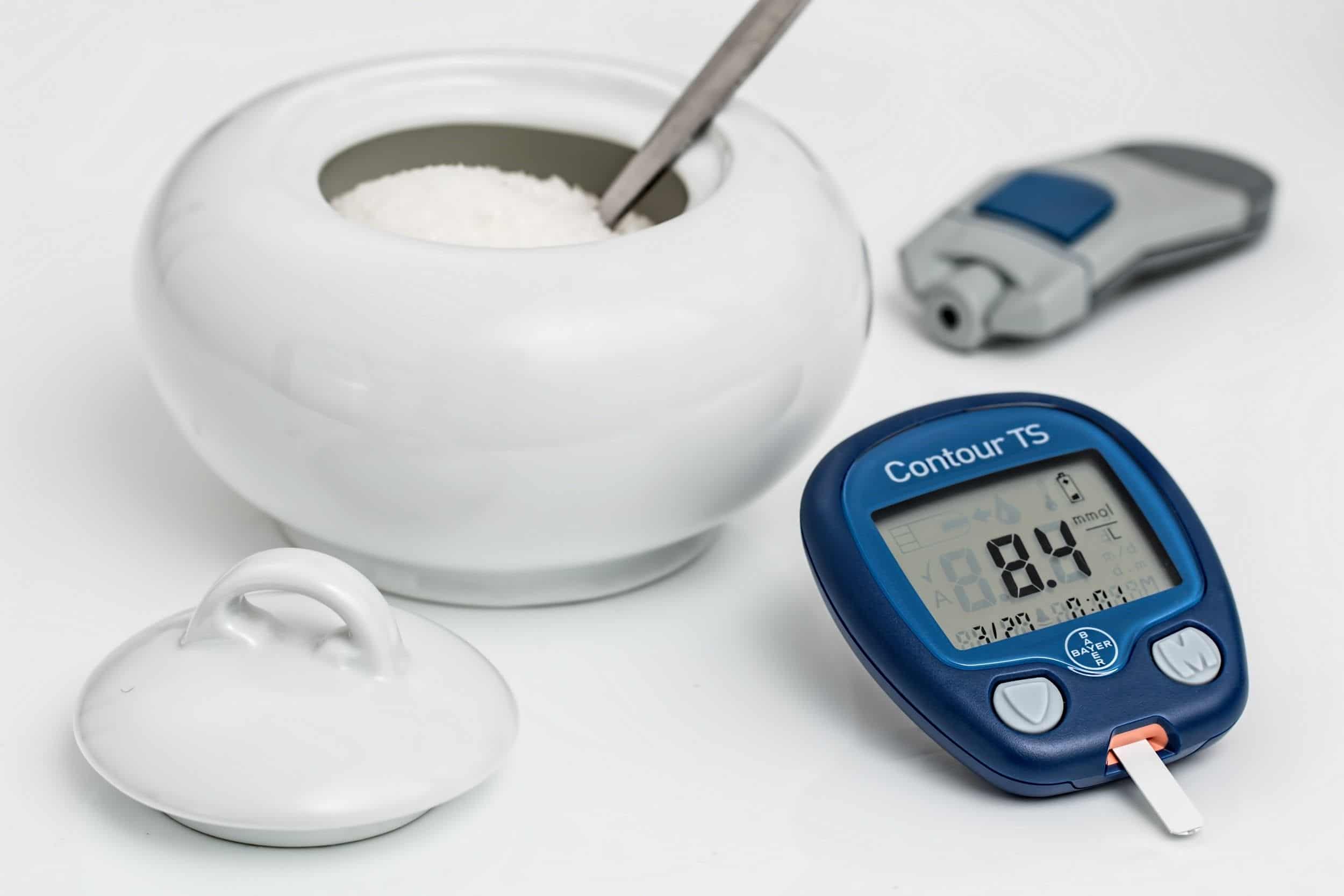
Insulin resistance can worsen if it’s unmonitored. Make sure you have a blood glucose meter with lancets and test strips to keep an eye on your glucose levels when you wake up, before meals, an hour after meals, and at bedtime. A normal fasting blood glucose reading is between 71 and 140 milligrams per deciliter (mg/dL). Anything lower is hypoglycemia, and anything higher is hyperglycemia, both of which are dangerous.
What Causes Fluctuations?

A few things can cause your blood glucose to spike, such as:
- Eating too many carbohydrates, especially the simple ones
- Eating very large meals
- Skipping your medication
- Not exercising
- Stress, pain, and other illnesses
- Sunburn
- Skipping breakfast
- A lack of sleep
- The dawn phenomenon (your blood glucose levels spike around 3:00 AM)
- Dehydration
- Menstrual cycles
- Steroids and antipsychotic medication side effects
Certain things also cause hypoglycemia, such as:
- Not eating enough or missing meals

- Reducing your carbohydrate intake too much
- Alcohol
- Taking too high of a dose of your diabetic medication
- Too much physical activity (exercise routines should always be discussed with your doctor)
- Side effects from other medications
- Hormone deficiencies
Quick Balancing Acts
Blood glucose that’s too high or low can cause serious complications, so you want to restore balance. Some ways to bring blood glucose down fast are:
- Drink two glasses of water
- Exercise
- Drink green tea
- Drink black coffee
- Seek medical attention if levels remain high

What to do if your blood glucose is too low:
- Eat or drink something with fast-acting sugar, albeit a small amount
- Wait 10 minutes
- Test your glucose again
- Seek medical attention if your levels remain low
Two Main Homecare Reminders
Two changes in your daily life can help you maintain better control and even reverse the condition. Remission isn’t a cure; it’s the temporary reversal of a condition, and it’s up to you to keep it that way.
Maintaining Weight Loss
Weight loss is the best management strategy for T2D. Evidence suggests that it can cause remission in diabetic patients, but remission is temporary and controlled by your daily lifestyle, which means that you need to maintain the weight loss. A longitudinal study of 33,184 participants over 23 years was published in the BMC Public Health Journal. The subjects were all at high risk of developing T2D, and the majority of their body mass indices (BMIs) were nearly normal at 25. Over the years, those who didn’t maintain their BMI had an increase in their risk for diabetes. The risk increased by between 1.04 and 1.06% every time the participants gained one percent of their body weight.
Weight maintenance is associated with better management. The accumulation of fat around the liver and pancreas leads to your beta cells not working properly, which could cause insulin resistance or the eventual need for insulin. A review by Newcastle University examined the likelihood of staying in remission with fast weight loss and maintenance. According to the review, many diabetics lose weight, but they quickly regain it over the first year. This yo-yo effect doesn’t decrease the long-term risks of the condition returning.
According to the Diabetes Remission Clinical Trial (DiRECT), maintenance should follow a loss of 33 pounds. Using a low-calorie diet with physical activity helps you melt the fat around your liver and pancreas, but maintaining it requires you to stick to a healthier lifestyle and avoid returning to old habits. Participants of numerous studies in the review were more successful in long-term remission when they maintained their weight loss. Some of them maintained remission for 5 and 10 years. Don’t simply aim to lose weight; use diabetic-friendly lifestyle changes to keep your risk at bay. 
Psychological Battle
Finding out that you have a lifelong condition takes its toll on your psychological well-being. Stress is natural when you don’t know how to manage your condition or reverse it. Unfortunately, the stress hormones cortisol and adrenaline aggravate T2D. They cause uncontrollable fluctuations in blood glucose, impair glucose and insulin tolerance, and activate fat cells. Stress even pushes your blood pressure up, causing your risk for heart disease to increase. The only way to avoid this is by dealing with your stress daily. Some useful methods to reduce stress include:
- Journaling
- Meditation
- Mindfulness
- Socializing
- Exercise
- Laughing more
- Learning more about diabetes
- Eating healthier
- Sleeping better
- Talking to a professional
- Removing stress triggers
- Practicing progressive muscle relaxation (PMR)
- Using breathing exercises
- Organizing your days
- Taking a nature walk
- Hugging someone

- Getting a new hobby
- Setting SMART goals
- Adopting optimism
- Practicing positive self-talk
- Expressing gratitude
- Joining a yoga class

Living under stress only makes the battle harder. Adopt a few new habits to counteract the consequences of uncontrolled T2D.
Food For Thought
Managing your T2D at home is simple with the right knowledge, weight loss to keep your condition under control, and stress-reducing techniques to make your days a little easier.
If you would like to receive a free resource sheet to help you take control of diabetes, click the button below to receive your gift.
I wanted to talk about this topic because it is absolutely possible to prevent and even reverse Type 2 Diabetes (but you cannot reverse Type 1). Yes, it’s possible! and emerging studies looking at lifestyle medicine and prevention support this! But I always tell my patients that you must be dedicated and diligent in adopting a healthy lifestyle to get the best results. You can create certain behaviors and practices that will not only enrich your life, but that you can pass on to your family, friends, and community, to help break the cycle of this chronic disease so that you can leave a legacy of health to your loved ones.
I use functional medicine and lifestyle medicine as the first line of treatment, before medications, to treat lifestyle-related chronic diseases. Lifestyle-related chronic diseases include diabetes, hypertension, obesity, and some cancers, just to name a few. Lifestyle practices, such as eating a low glycemic, whole-food plant-based diet and regular physical activity, can help you improve your blood sugar levels, maybe reverse type 2 diabetes. In certain cases, these approaches may even outperform pharmaceutical therapy.
But I always tell my patients that conventional medications may be appropriate at this time to prevent catastrophic illness, but over time, you can work to make the necessary lifestyle changes to possibly reduce and/or eliminate medications. Please remember to always consult your physician for your particular needs and circumstances prior to making any decisions whatsoever.
Is Dietary Supplementation Right For You?
When it comes to managing your blood sugars (in general), pre-diabetes, and diabetes, there are many things that you can do to help control your blood sugar levels. One important aspect is diet. What you eat affects your blood sugar, so it’s important to be mindful of what goes into your body.
But it is very important to note that we are not eating the same foods we ate years ago because the soils have been depleted of critical nutrients through current industrial farming practices. And because the soil is not as good as it used to be, the food supply (grown from the depleted soil) is not as good as it used to be. For example, you are not getting the same levels of chromium and magnesium as you would have gotten 30 or even 50 years ago.
Second, much of the food has been processed and genetically altered, which can impact the inherent and unique nutritional composition that each food possess. For example, ancient einkorn wheat has less gluten, more protein, more Vitamin A, and more beta carotene, than modern genetically modified wheat.
Third, the toxic load in the environment today is much higher than 100 years ago. We can see this with global warming, toxic landfills, polluted oceans and waterways, etc. Toxicity levels interfere with nutrient assimilation and absorption not just into the foods, but into our bodies as well. We often see elevated blood sugar levels with poor nutrition and toxicity.
In addition to diet, there are dietary supplements that can have an impact on blood sugar levels. Dietary supplements for diabetes are becoming increasingly popular as people look for ways to improve their blood sugar control.
For some people, vitamin and mineral supplements offer important health benefits. Supplements are designed to fight deficiencies found in our diet and complement the food we eat regularly. Supplements are basically “helping hands” to our daily food.
If you suspect that you aren’t getting the nutrients you need, consider shifting your focus from supplements to eating better.
And if you are unable to eat better, the supplements in my Blood Sugar Support Bundle may provide the extra boost you need.
These are my favorite Diabetes Prevention Supplements to use! This Blood Sugar Support Bundle will ensure you have the intake of the important vitamins, minerals, and probiotics to decrease inflammation and boost your innate wellness day and night. Taken together, it’s a solid plan for increasing your body’s natural resiliency while encouraging healthy blood sugar levels.
For best results make sure you use these supplements with dietary changes including a whole food plant-based diet, regular exercise (at least 2-3x per week), regular sleep (8 hours per night), and intermittent fasting (at least 1-3x per week).
It’s important to note that supplements are NOT a replacement for your regular medication regimen prescribed by your doctor. However, they can be used in addition to help manage your blood sugar levels.
Supplements have the potential to interact with diabetes medications, so it’s important to speak with a healthcare provider before starting any new supplement regimen. Have you tried any dietary supplements for your diabetes? Share your experience in the comments below!
Tools For Diabetes Prevention and Monitoring
Blood Sugar Monitoring
As you know, I always stress the importance of taking control of your health. Monitoring your blood sugar levels is one of the best ways to do this. To do this, a single drop of blood is collected with disposable lancets and placed on a disposable test strip, which you insert into a home blood-sugar monitoring device, called a glucometer.
The common times for checking your blood sugar are when you first wake up (fasting), before a meal, 2 hours after a meal, and at bedtime; however, you should check your blood sugar as many times a day as your health care team suggests.
Monitoring your blood sugar level provides you and your doctors with important knowledge about how food, activity, medication, stress, and other elements might affect your blood sugar levels. This data will assist you and your doctor in developing a therapy plan that is suited to your demands.
There are several types of blood glucose meters, lancets, and test strips to choose from. I often recommend this glucometer, lancets, and test strips.
Weight Monitoring
Since weight management is very important in combatting chronic diseases such as diabetes, I recommend that you be mindful of your weight and its fluctuations, and that you monitor your weight AT LEAST on a weekly basis. I recommend a scale that includes a body composition monitor (*this scale cannot be used with a pacemaker or other implanted devices).
Physical Activity
Physical activity (or exercise) can improve your health and reduce the risk of developing several chronic diseases like high blood pressure, type 2 diabetes, and cancer, just to name a few. Physical activity actually improves insulin sensitivity. Physical activity can improve your mood, boost your immune system, and even help you maintain a healthy weight.
I often recommend yoga and resistance training for physical activity, but as you are aware, there are plenty of forms of “movement” that you can do! But for the basics, especially if you’re just getting started, yoga and resistance training are where I would start.
Yoga
Yoga can be a great way to improve your strength and flexibility, manage your stress, improve your heart health, and lose weight! I recommend using this yoga mat to get started with your yoga practice today!
Resistance Training
Resistance training is the mainstay for overall health. It not only has beneficial effects on reducing body fat, it also increases muscle size and strength. Here are some basic resistance bands that I recommend to everyone. They are great for physical therapy, yoga, strength training, and excellent for traveling.
Food!
Remember, living a healthy lifestyle including eating a whole foods plant-based diet and regular physical activity are the best ways to prevent diabetes.
The Diabetes Meal Plan is geared towards those people with diabetes or prediabetes. The foods are moderately low in carbs, low glycemic, fiber rich, and contain a balance of nutrients to help prevent blood sugar spikes and dips. Foods are also included that may help to lower blood sugar.
Please talk with your doctor about any complementary health approaches, including supplements, you use.
Dr. Nicolle Martin
Some of the links in this article are "affiliate links", a link with a special tracking code. This means if you click on an affiliate link and purchase the item, we will receive an affiliate commission.
The price of the item is the same whether it is an affiliate link or not. Regardless, we only recommend products or services we believe will add value to our readers.
By using the affiliate links, you are helping support our Website, and we genuinely appreciate your support.
Last updated on January 28th, 2022 at 06:59 am

Minimize Medications. Maximize Health.
Are you super busy but need to take control of your health? Are you tired of being tired? Subscribe to my “Minimize Medications, Maximize Health Blog” and I’ll give you 7 Tips to Get Healthy in No Time absolutely FREE.







